If you have ever felt unwell after eating a specific meal, you might have quickly assumed you have a food allergy. It is a reasonable assumption, yet often incorrect.
Digestive discomfort is incredibly common, but the biological mechanisms behind your symptoms matter significantly. Confusing a food intolerance with a food allergy is a frequent occurrence, largely because the symptoms often overlap. However, the difference between the two is crucial for your long-term health and safety.
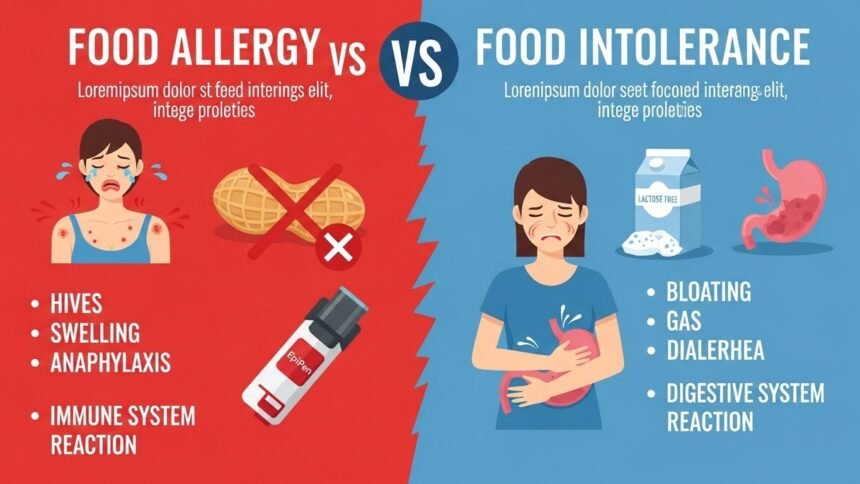
A true food allergy involves the immune system and can be life-threatening. A food intolerance, while uncomfortable and disruptive to your quality of life, generally involves the digestive system and is rarely dangerous.
Understanding the distinction helps you manage your diet effectively and seek the correct medical advice. This article explores the causes, symptoms, and management strategies for both conditions.
The Core Difference: Immune vs. Digestive
To understand the difference, we must look at how the body reacts biologically.
What is a Food Allergy?
A food allergy is an immune system reaction. When you have an allergy, your immune system mistakenly identifies a specific food protein as harmful. In response, it produces antibodies called Immunoglobulin E (IgE) to fight off the invader.
The next time you consume even a microscopic amount of that food, these antibodies signal your immune system to release chemicals, such as histamine, into your bloodstream. This chemical release causes the allergic reaction.
According to Allergy UK, symptoms can affect different areas of the body simultaneously, including the skin, respiratory system, and cardiovascular system.
What is a Food Intolerance?
A food intolerance usually occurs in the digestive system. It typically means your body lacks the specific enzymes needed to break down certain foods properly, or you are sensitive to certain food additives or chemicals.
Unlike an allergy, an intolerance does not involve the immune system (with the exception of Coeliac disease, which is an autoimmune condition, not a standard allergy or intolerance). People with an intolerance can often eat small amounts of the offending food without severe trouble.
Here is a quick comparison to help you distinguish between the two:
| Feature | Food Allergy | Food Intolerance |
|---|---|---|
| System Involved | Immune System | Digestive System |
| Onset of Symptoms | Immediate (minutes to 2 hours) | Delayed (30 minutes to 48 hours) |
| Amount Consumed | Tiny trace amounts trigger reaction | Reaction often depends on portion size |
| Severity | Can be life-threatening (Anaphylaxis) | Uncomfortable but rarely dangerous |
| Common Symptoms | Hives, swelling, difficulty breathing | Bloating, gas, diarrhoea, stomach pain |
Common Causes and Factors
Identifying the trigger is the first step toward relief. While any food can cause a reaction, specific culprits are more common than others.
Causes of Food Intolerance
Food intolerance is often multifactorial. The Mayo Clinic notes several primary causes:
- Absence of an enzyme: To digest foods fully, you need enzymes. The most common example is lactose intolerance, where the body lacks lactase, the enzyme required to digest milk sugar (lactose).
- Chemical causes: Some people are sensitive to natural chemicals in food, such as amines in aged cheeses or caffeine in coffee.
- Food poisoning: Sometimes, a reaction is caused by naturally occurring bacteria or toxins in spoiled food (like histamines in fish that hasn’t been stored correctly).
- Additives: Artificial colours, preservatives like sulphites (often found in dried fruit or wine), and flavour enhancers like MSG (monosodium glutamate) can trigger intolerance reactions.
- FODMAPs: Certain fermentable carbohydrates can cause significant distress in people with Irritable Bowel Syndrome (IBS). You can read more about this on Healthline.
Causes of Food Allergies
While over 170 foods have been reported to cause allergic reactions, a small group accounts for the vast majority of cases. In the UK, food businesses must declare 14 specific allergens by law.
The most common allergic triggers include:
- Peanuts and tree nuts (walnuts, almonds, cashews)
- Shellfish (shrimp, crab, lobster)
- Fish
- Milk
- Eggs
- Soy
- Wheat
Symptoms: What to Look For
Because the symptoms of intolerance and allergy often overlap—specifically regarding stomach pain—it can be difficult to tell them apart without medical testing. However, the severity and location of symptoms provide clues.
Symptoms of Food Intolerance
Symptoms of food intolerance generally rise slowly and are mostly confined to the gastrointestinal tract. They may include:
- Excessive gas and bloating
- Abdominal pain or cramping
- Diarrhoea
- Nausea
- Heartburn
- Headaches or migraines (specifically with histamine or tyramine intolerance)
Crucially, the severity of these symptoms usually correlates with how much of the food you ate. If you are lactose intolerant, a splash of milk in tea might be fine, but a milkshake could cause distress.
Symptoms of Food Allergy
Allergic reactions happen quickly. Symptoms can range from mild to severe and may include:
- Tingling or itching in the mouth
- Hives, itching, or eczema
- Swelling of the lips, face, tongue, and throat
- Wheezing, nasal congestion, or trouble breathing
- Abdominal pain, diarrhoea, nausea, or vomiting
- Dizziness, lightheadedness, or fainting
In severe cases, a food allergy can cause anaphylaxis, a life-threatening reaction that requires immediate medical attention. This involves a sudden drop in blood pressure and constriction of airways.

Diagnosis: Getting the Right Answers
Self-diagnosis can be risky. If you suspect you have a food issue, consulting a GP is essential. They may refer you to an allergy specialist or a dietitian.
Diagnosing Allergies
Doctors typically use a combination of history taking and clinical tests:
- Skin Prick Test: A tiny amount of the allergen is placed on your skin, which is then pricked. If a raised bump (hive) appears, you are likely allergic.
- Blood Test: This measures the amount of IgE antibodies in your blood specific to certain foods.
Diagnosing Intolerances
Diagnosing a food intolerance is trickier because there are fewer reliable clinical tests. The British Dietetic Association warns against unproven commercial tests (like hair analysis or IgG blood tests) which have no scientific basis.
The gold standard for diagnosing intolerance is the Elimination Diet. This involves:
- Removing suspected foods from your diet for a period (usually 2–6 weeks).
- Monitoring symptoms to see if they improve.
- Gradually reintroducing foods one by one to pinpoint the culprit.
Breath tests are also available for specific conditions, such as lactose or fructose intolerance, to measure how well you digest sugars.
Treatment and Management
Once you have identified the issue, management depends entirely on whether it is an allergy or an intolerance.
Managing Food Allergies
The only effective management for a food allergy is strict avoidance. Even trace amounts can trigger a reaction.
- Read Labels: You must become an expert at reading ingredient lists. In the UK, the Food Standards Agency mandates that allergens be emphasised (usually in bold) on pre-packed food.
- Emergency Medication: People with severe allergies usually carry an adrenaline auto-injector (EpiPen or Jext) at all times.
- Communication: When dining out, you must clearly inform staff of your allergy.
Managing Food Intolerance
Management of food intolerance is more flexible. The goal is often symptom reduction rather than total avoidance.
- Determine Your Threshold: You may be able to handle small amounts. Trial and error will help you find your limit.
- Enzyme Supplements: Over-the-counter lactase tablets can help those with lactose intolerance digest dairy products. Similar enzymes exist for bean digestion (alpha-galactosidase).
- Dietary Modification: Swapping specific foods for alternatives (e.g., almond milk instead of cow’s milk) is the primary strategy.
- Addressing Gut Health: Sometimes, intolerances are secondary to other gut issues. Improving your microbiome might help. Harvard Health suggests that a diverse diet supports better gut flora.
Practical Tips for Daily Life
Living with dietary restrictions requires planning, but it becomes second nature over time. Here are some practical tips to navigate daily life safely.
1. Keep a Food and Symptom Diary
Before seeing a doctor, track your intake. Write down everything you eat, the time you ate it, and any symptoms that follow. Patterns often emerge that you might miss otherwise. For example, you might notice that you only feel bloated after eating pasta and bread, pointing toward a wheat intolerance or Coeliac disease.
2. Cook from Scratch
Processed foods are often hidden sources of allergens and FODMAPs (such as onion and garlic powder). Cooking from scratch gives you total control over ingredients. Using fresh herbs and spices allows you to create flavour without relying on pre-made sauces that may contain additives.
3. Be Wary of “Free-From” Cross-Contamination
If you have a severe allergy, simply ordering a “gluten-free” dish in a restaurant might not be enough if the kitchen uses the same frying oil for breaded items. Always ask about cross-contamination policies. The NHS provides excellent guidance on managing this risk.
4. Understand Histamine Build-up
For some, the freshness of food matters. Foods high in histamine (like aged cheeses, fermented foods, and leftover meat) can trigger intolerance symptoms. If you suspect histamine intolerance, try freezing leftovers immediately rather than keeping them in the fridge. Research from the National Institute of Health suggests low-histamine diets can significantly reduce symptoms for sensitive individuals.
5. Check for Hidden Lactose
Lactose isn’t just in milk. It is often used as a filler in processed meats, crisps, and even some medications. If you are highly sensitive, checking the fine print is vital. The NIDDK offers comprehensive advice on hidden sources of lactose.
The Bottom Line
While the terms are often used interchangeably, food intolerance and food allergy are distinct conditions with different risks.
A food allergy is an immune response that can be dangerous and requires strict avoidance. A food intolerance is a digestive response that causes discomfort but is generally manageable through dietary adjustments and moderation.
If you constantly feel unwell after eating, do not guess. Persistent digestive symptoms can also indicate other conditions like Irritable Bowel Syndrome (IBS) or Inflammatory Bowel Disease (IBD). By working with a healthcare professional to identify your specific triggers, you can reclaim your relationship with food and eat without fear or discomfort.