If you or a loved one has been struggling with unexplained lung or liver issues, your doctor may have mentioned Alpha-1 testing. While the name might sound complex, the process is actually quite straightforward. This simple screen can provide the answers needed to manage your health effectively and take proactive steps for your future.
Alpha-1 Antitrypsin Deficiency, often abbreviated as AATD, is a genetic condition that can lead to serious health complications if left undiagnosed. Despite being one of the most common inherited disorders, it remains significantly underdiagnosed. At its core, Alpha-1 testing is the key to unlocking a personalised care plan and improving long-term outcomes.
What Is Alpha-1 Antitrypsin Deficiency?
Alpha-1 Antitrypsin (AAT) is a protein produced primarily in the liver. Its main job is to travel through the bloodstream to the lungs, where it protects the delicate lung tissue from damage caused by inflammation and environmental irritants. When someone has AATD, their body doesn’t produce enough of this protein, or the protein is “mispun” and gets stuck in the liver.
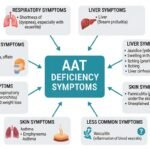
This deficiency often manifests as rare diseases that mimic more common ailments. Without enough protective protein, the lungs become vulnerable, often leading to chronic obstructive pulmonary disease (COPD) or emphysema at a much earlier age than usual—even in non-smokers. Additionally, the buildup of abnormal proteins can lead to significant liver disease, including cirrhosis or jaundice.
Why Is Alpha-1 Testing So Important?
The primary goal of Alpha-1 testing is early diagnosis. Because the symptoms of AATD—such as shortness of breath, wheezing, and chronic cough—are so similar to asthma or standard smoking-related COPD, many patients spend years without the correct diagnosis. Identifying the SERPINA1 gene mutation responsible for this condition allows healthcare providers to prioritise targeted treatments rather than generic therapies.
According to the World Health Organization, every individual diagnosed with COPD should be screened for Alpha-1 at least once. This is because knowing your “Alpha status” changes how doctors approach your lung function and overall wellness.
Who Should Consider Alpha-1 Testing?
You might be wondering if you should request a test. Medical experts at the Mayo Clinic and the European Respiratory Society suggest testing for anyone who meets the following criteria:
- People diagnosed with COPD, emphysema, or bronchiectasis.
- Individuals with unexplained liver disease, especially infants or adults with persistent jaundice.
- Those with a family history of AATD or early-onset lung issues.
- Adults with refractory asthma (asthma that doesn’t respond well to standard treatments).
- Individuals with a rare skin condition called panniculitis.
How the Testing Process Works
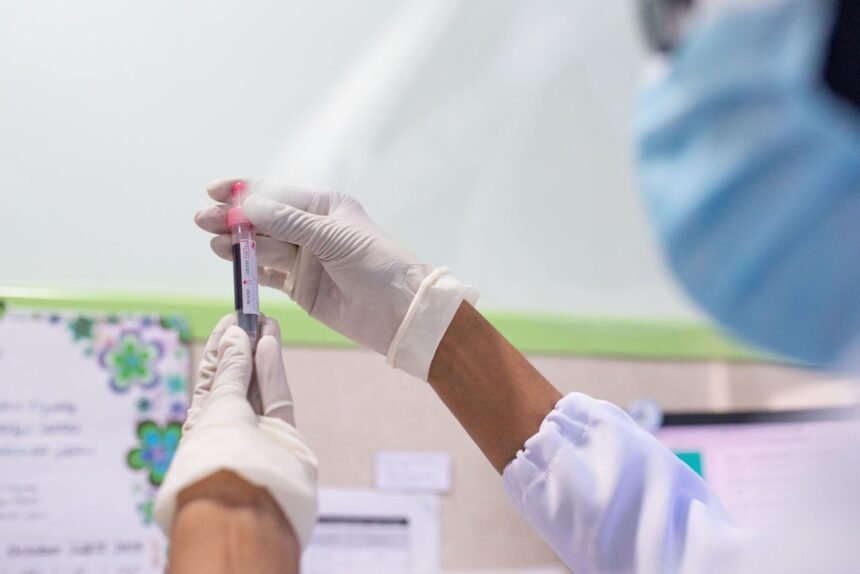
The actual Alpha-1 testing is usually performed via a simple blood test. There are three primary ways clinicians analyse your levels and genetics:
- AAT Level Test: This measures the concentration of the Alpha-1 protein in your blood. If levels are low, further genetic analysis is required.
- Phenotype Testing: This looks at the actual proteins in your blood to see how they are behaving and identifies which “Pi” (Protease Inhibitor) type you have.
- Genotyping: This examines your DNA for the most common mutations (the S and Z alleles).
In some cases, your doctor may recommend a full gene sequencing if common tests are inconclusive. Below is a comparison of what different Alpha-1 testing results might look like:
| Genotype | Description | Risk Level |
|---|---|---|
| PiMM | Normal Alpha-1 protein levels. | No increased risk. |
| PiMZ genotype | A “carrier” state; one normal gene, one abnormal gene. | Low to moderate risk, especially if smoking. |
| PiZZ | Most common severe form; two abnormal genes. | High risk for lung and liver disease. |
| PiSZ | Combination of two different mutations. | Increased risk for lung disease. |

What Happens After a Positive Result?
Receiving a positive result from Alpha-1 testing can feel overwhelming, but it is the first step toward taking control of your health. Knowledge is power. Once diagnosed, your medical team can monitor your lung function more closely through regular spirometry and imaging.
One of the most effective treatments for those with severe lung involvement is enzyme replacement therapy (also known as augmentation therapy). This involves weekly infusions of purified Alpha-1 protein to slow the progression of lung damage. You can find detailed research on the efficacy of these infusions via the Cochrane Library and PubMed Central.
It is also highly recommended to seek genetic counselling. Because this is an inherited condition, your children, siblings, and parents may also be at risk. A counsellor from an organisation like the Genetic and Rare Diseases Information Center (GARD) can help navigate these delicate family conversations.
Lifestyle Adjustments
Beyond medical intervention, lifestyle changes are crucial. If you test positive for AATD, you must:
- Avoid smoking or vaping entirely.
- Minimise exposure to secondhand smoke and industrial dust.
- Maintain a healthy weight to reduce stress on your liver and lungs.
- Limit alcohol consumption to protect your liver tissue.
In severe cases where the liver or lungs have sustained significant damage, more intensive interventions like a lung transplant or liver transplant may be discussed with specialists at centres such as the British Liver Trust or the Asthma + Lung UK foundation.
The Role of Clinical Research
The field of Alpha-1 research is rapidly evolving. From new gene-editing techniques discussed in Nature Genetics to innovative drug trials listed on ClinicalTrials.gov, there is more hope today than ever before. Staying informed through reputable journals like The Lancet Respiratory Medicine ensures you are aware of the latest breakthroughs.
Many patients also find solace and support through the Alpha-1 Foundation, which provides resources for both patients and healthcare professionals to improve the standard of care globally.
Frequently Asked Questions (FAQs)
Is Alpha-1 testing expensive?
Many organisations and pharmaceutical companies offer free or subsidised testing kits for those who meet the clinical criteria for COPD or unexplained liver disease. In the UK, the NHS typically covers the cost of the test if your GP or respiratory consultant deems it medically necessary. You can also find more info on WebMD’s lung health portal.
Can children be tested for Alpha-1?
Yes, children are often tested if they show signs of prolonged neonatal jaundice or other liver complications. However, genetic testing for asymptomatic children is a complex ethical decision and should always be discussed with a genetic counselling expert to weigh the pros and cons.
Does a positive test mean I will definitely get sick?
Not necessarily. While Alpha-1 testing identifies a genetic predisposition, many people with certain genotypes (like PiMZ or even some PiZZ individuals) lead long, healthy lives. Factors like environment, smoking status, and early diagnosis play a massive role in determining the severity of the condition.
Can I get tested at home?
There are “finger-prick” dry blood spot tests available that can be posted to a laboratory. While convenient, it is always best to have Alpha-1 testing overseen by a medical professional who can accurately interpret the results and provide the necessary follow-up care and support.